The EFP thanks Sunstar for its support and its unrestricted grant
Perio and Diabetes overview
Both gum diseases and diabetes are pervasive, systemic conditions with numerous interactions and impact on our overall health. About 80% of people aged over 35 suffer from some kind of gum problem and about 7% of the population suffers from diabetes, although in many cases this goes undiagnosed.
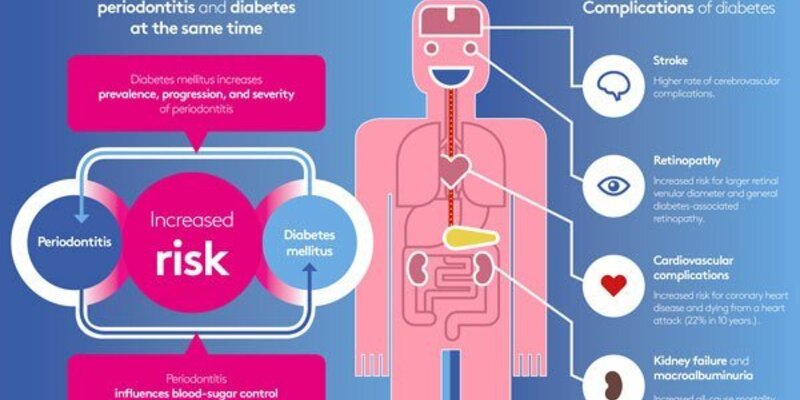
There are strong associations between the two diseases. Indeed, there is a two-way (bidirectional) relationship between periodontal disease and diabetes. This means that people with periodontitis have a higher risk of diabetes and patients with diabetes are three times more likely to develop periodontal disease.
Our Perio & Diabetes campaign explains the links between periodontal diseases and diabetes mellitus and the actions that can be taken in terms of prevention, treatment, and management.
The EFP thanks Sunstar for its unrestricted grant that has made possible the creation of Perio & Diabetes.
- Brochure for patients and the public
- FAQs
- People with periodontitis are likely to develop diabetes mellitus – and vice versa
- Periodontal treatment for people with diabetes
- Recommendations for patients and the public
- Recommendations for policymakers
Check our animations in nine different languages!
English
French
Japanese
Azerbaijani
Italian
Portuguese
Chinese
German
Spanish
Scientific report
The Perio & Diabetes project has been created from evidence-based science and the conclusions of the Perio-Diabetes Workshop held by the EFP and the International Diabetes Federation, in partnership with Sunstar, in Madrid in February 2017.
All the materials provided here – the recommendations, the graphic and video material, the scientific reports – have been created by an expert team based on the detailed scientific papers produced by this workshop and published in the EFP’s Journal of Clinical Periodontology.
Meet the Perio & Diabetes experts
For media
If you are a journalist and would like more information about this campaign, please contact press@efp.org