Classification & Guidelines, Clinical & Translational Research, Article
How patient-reported outcomes should be included in periodontology and implant dentistry
16 March 2026
Patient-reported outcomes are increasingly important in periodontology and implant dentistry, particularly in relation to aesthetic factors. Last year’s focused workshop organized by the EFP with the Spanish and Italian societies of periodontology (SEPA and SIdP) examined the latest evidence in this area. José Nart (SEPA) and Francesco Cairo (SIdP) address patient-related outcomes in relation to gingival-recession defects, implant timing, and the management of peri-implant soft-tissue complications, while David Herrera (chair, EFP workshop committee) discusses the implications of the workshop’s consensus report for future research and clinical practice, and Moritz Kebschull (EFP past president) considers the forthcoming clinical-practice guideline that will be informed by this report.
Gingival-recession defects, implant timing, and the management of peri-implant soft-tissue complications
By José Nart and Francesco Cairo
Gingival recession defects
Regarding the treatment of single or multiple gingival recessions, a high level of evidence suggests that various procedures can achieve excellent clinical and aesthetic outcomes. Of the different procedures explored at the workshop, it was connective-tissue graft techniques that were shown to provide better root-coverage outcomes.
Surgical therapy was found to have a positive effect on both clinician-reported aesthetic scores and patient-reported aesthetic perception and satisfaction. The conclusions of the workshop recommended a clear definition of the professional and patient perspectives in each clinical scenario, along with a clear assessment of the cost-benefit ratio and morbidity of each selected procedure.
Surgical treatment for root coverage of single recession had a positive effect on both clinician-reported aesthetic scores and patient-reported aesthetic perception and satisfaction. Bilaminar techniques—mainly applying a connective-tissue graft (CTG) under a coronally advanced flap (CAF)—are generally associated with higher outcomes.
Interestingly, aesthetic outcomes rated by clinicians may not always correspond to patient opinion, with patient satisfaction not necessarily influenced by the amount of root coverage. Reasons for this differing perspective between clinicians and patients may include clinicians’ high level of sensitivity in evaluating the complete root coverage as the treatment goal, while they consider soft-tissue characteristics (such as colour and scar-tissue persistence) to be secondary outcomes. Conversely, patient satisfaction seems to be strongly influenced by the final soft-tissue integration, irrespective of the amount of root coverage. This means that patients may be likely to be satisfied by partial root-coverage outcomes when the final soft-tissue aesthetics are very pleasing.
These elements may explain, at least in part, the observed discrepancy between clinician and patient perceptions.
Immediate versus early/delayed implant placement
On the timing of implant placement, the available evidence suggests that patient-reported outcomes—such as satisfaction, comfort, aesthetics, and quality of life—are generally favourable across immediate, early, and delayed protocols, when these procedures are appropriately indicated and executed.
Immediate implant placement may offer perceived advantages related to reduced treatment time and fewer surgical interventions, which some patients value highly. But expectations, aesthetic demands, and individual risk profiles play a critical role in shaping the patient experience. The workshop emphasized the need for clear communication and shared decision-making to align treatment choice with patient preferences and expectations.
In dental implant procedures, the addition of a CTG immediately after implant placement significantly mitigated the apical shift in the mid-facial mucosal level. Soft-tissue augmentation procedures are recommended at immediate implant placement in the presence of a thin phenotype and when a minor buccal bone dehiscence is present.
However, most of these soft-tissue augmentation procedures are not perceived by patients.
The existence of a localized gingival recession or a buccal position of the tooth in relation to the alveolar process might be contraindications for immediate implant placement.
There is no preference on the timing of soft-tissue volume augmentation during dental implant therapy (early, delayed, or late) according to the existing evidence.
Treatment of peri-implant buccal soft-tissue dehiscences
In the management of peri-implant buccal soft-tissue dehiscences, patient-reported outcomes were shown to be strongly influenced by aesthetic concerns, morbidity, and the burden of additional surgical procedures. Surgical correction can improve patient satisfaction—particularly in the aesthetic zone—but may also be associated with increased discomfort and longer recovery. The workshop highlighted the limited but emerging evidence on patient-reported outcomes in this area and underscored the importance of prevention, minimally invasive approaches, and realistic patient counselling regarding achievable outcomes.
In the treatment of peri-implant dehiscences, soft-tissue augmentation using a CTG beneath a CAF resulted in favourable outcomes in both clinician- and patient-perceived aesthetics. The connective-tissue graft remains the leading treatment material for achieving the highest amount of soft-tissue thickness, keratinized mucosa, and dehiscence coverage. The graft should have dense connective tissue predominantly comprising lamina propria. In terms of the techniques, both CAF and the alternative approach of tunnelling plus CTG improve the outcomes of peri-implant soft-tissue dehiscences (PSTD). However, the choice depends upon site conditions and surgical expertise.
Modifying the prosthetic component prior to the surgical procedure is often required to allow space for the tissue and even papillae. In clinical practice, such decisions are made based on individual site-specific circumstances.
Conclusions
Overall, the workshop emphasized that patient-reported outcomes are a critical component of evidence-based periodontal and implant dentistry. Future research should prioritize standardized patient-reported outcome measures and long-term patient perspectives to better inform clinical decision-making and optimize patient-centred care.
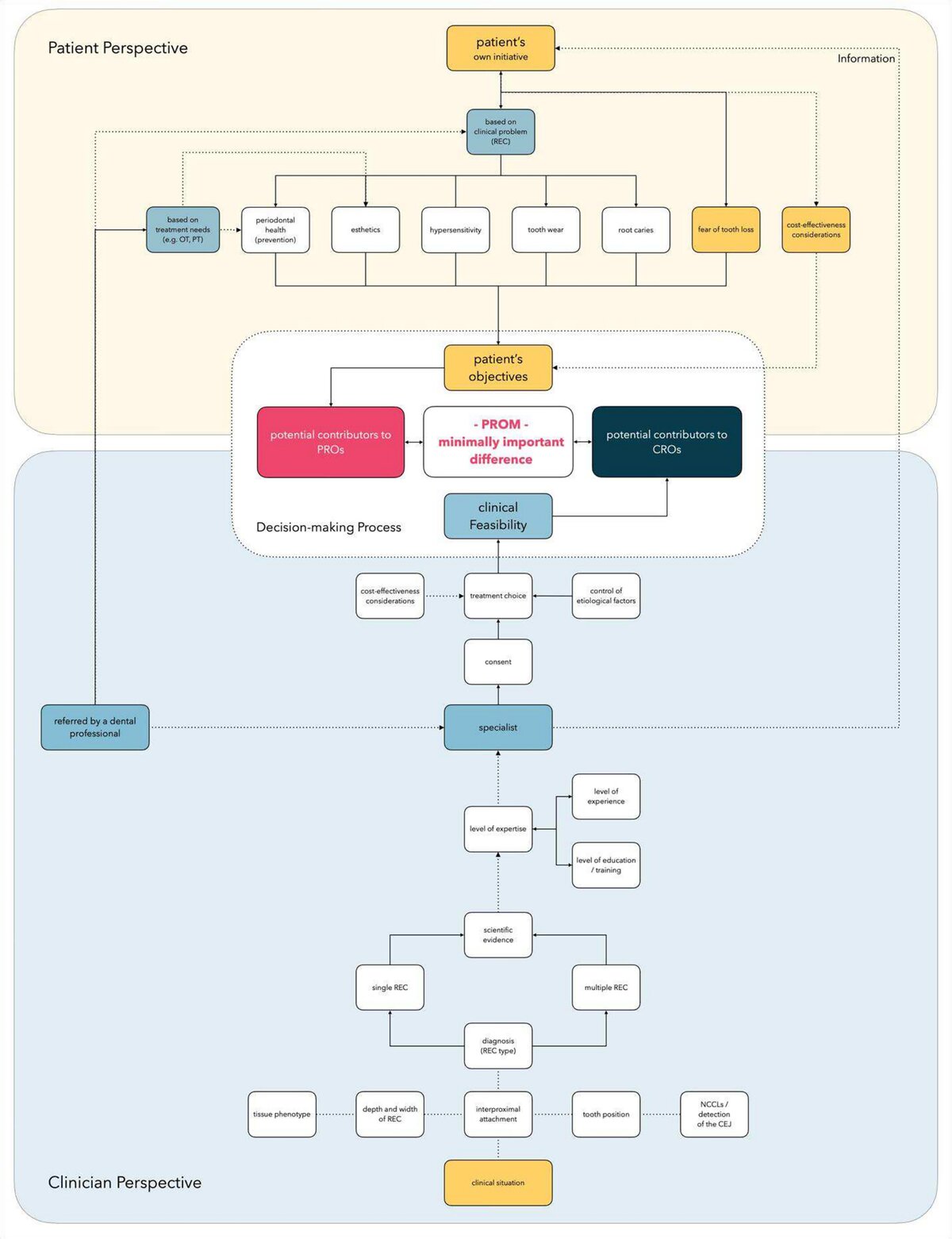
CROs, clinician-reported outcomes; NCCLs, non-carious cervical lesions; OT, orthodontic treatment; PROMs, patient-reported outcome measures; PROs, patient-reported outcomes; PT, prosthodontic treatment; REC, gingival recession. Colour code: blue boxes, clinically/clinician-related factors; yellow boxes, patient-related factors.
From: Tonetti, M., M. Sanz, F. Cairo, et al. 2025. “Aesthetics and Patient-Reported Outcomes in Periodontology and Implant Dentistry: Consensus Report.” Journal of Clinical Periodontology vol. 52, no. 9: 1222–1244. https://doi.org/10.1111/jcpe.14182.
Implications of the focused workshop’s consensus report
By David Herrera
When the focused workshop on aesthetics and patient-reported outcomes (PROs) was initially proposed, it was under the assumption than the target people for the different interventions needed to be more involved in the decision-making process and in the evaluation of the outcomes.
While this may be true for all types of interventions in medicine, it is even more important when the indications include an improvement—or, at least, limiting any negative impact—of aesthetics.
The initial analysis to be made was if what the patient perceives as a successful intervention aligns with the evaluation of the clinician and with the criteria used in the studies to define success. So, it is worth approaching the issue from these three perspectives: patient, clinician, and researcher.
For the patient, it must be highlighted that a true endpoint is a clinically meaningful one that reflects “how a patient feels, functions, or survives”, according to Stuart G. Baker in 2018[1]. Most outcomes routinely used in periodontology are surrogate outcomes, whose relevance to the patient is limited. Therefore, specific PROs should be developed, and they should be developed with patients rather than for patients, which will give them greater relevance to patients. The PROs can therefore be more informative than surrogate clinical outcomes in helping patients make decisions about their care.
For the clinician, clinician-reported outcomes (CROs) are essential for assessing the feasibility and efficacy of surgical procedures, including changes in tissue
phenotype features or the dimensions of a recession. Understanding which procedures are more efficacious and predictable will allow the selected PROs to evaluate their effectiveness in delivering real patient benefits to aid decision-making. Healthcare costs will also impact these choices.
For the researcher, the consensus report concluded that there is a need to develop, test, and validate optimized tools for measuring the benefits of surgical interventions, understanding the perspectives of clinicians and patients. It was considered as unlikely that most available outcomes and tools are valid or sufficiently sensitive to detect differences. For the development of specific PROs, patients with previous experience and a multidisciplinary team—combining those with expertise and experience in research, soft-tissue surgery, health psychology and biostatistics—will be required. Transcultural, socio-economic, and chronological factors may influence patients' perception of the benefits of a therapy, so these should always be kept in mind.
The consensus report of the workshop—published in the September 2025 issue of the Journal of Clinical Periodontology—will guide clinicians in understanding how to include patient-centred considerations, aiming to identify the best interventions in different clinical scenarios from the perspectives of both the clinician and patient.
In addition, the report will guide researchers in designing their studies, ensuring that the proper patient-reported outcomes are included and that the appropriate patient-reported outcome measures are implemented.
The consensus report not only emphasizes the importance of including patient-reported outcomes in research, but also outlines what could be the appropriate measures for assessing them in the three selected clinical scenarios: root-coverage surgical procedures for the treatment of single or multiple recessions, the treatment of soft-tissue dehiscences at dental-implant sites, and different reconstruction modalities for soft tissues post-extraction and for delayed implant placement.
[1] Baker, S. G. (2018). Five criteria for using a surrogate endpoint to predict treatment effect based on data from multiple previous trials. Statistics in Medicine, 37(4), 507-518. doi:10.1002/sim.7561.

How the workshop’s conclusions will help shape the new guideline
By Moritz Kebschull
The focused workshop on aesthetics and patient-reported outcomes, a joint initiative of SEPA and SIdP held under the umbrella of the EFP, represents a new and exciting way of working within European periodontology. By enabling our esteemed national societies to convene targeted workshops that address specific knowledge gaps, we can harness the collective expertise of our community in a highly focused manner, and feed the results directly into the EFP's formal guideline development process.
This is precisely what will happen at the 22nd European Workshop on Periodontology, scheduled for November 2026 at La Granja de San Ildefonso in Spain, which will develop an S3-level clinical practice guideline for the management of gingival recession. The guideline—the fifth EFP guideline after stage I-III and stage IV periodontitis, peri-implant diseases, and the yet-to-be-published one on gingival diseases—will be based on a series of commissioned systematic reviews and will follow a formalized, multidisciplinary consensus process, which is the hallmark of the EFP's rigorous approach to evidence-based guidance.
A key element of any clinical-practice guideline is the careful selection and prioritisation of outcomes. For gingival recession, this means defining not only the clinical endpoints that matter—such as root coverage and keratinized tissue width—but also those outcomes that matter most to patients, including aesthetics, sensitivity, and overall satisfaction.
This is where the focused workshop's findings become invaluable. By first establishing which patient-reported outcomes are most relevant and how they should be measured, we have laid the groundwork for a more meaningful interpretation of the evidence when the European Workshop on Periodontology convenes. A dedicated session at the workshop will use these insights, alongside a new systematic review of reported outcome measures, to formally define the importance of each outcome. This is a step that directly shapes the strength and direction of the guideline's recommendations.
This staged approach of first understanding the patient perspective through a focused workshop and then integrating those findings into the broader guideline process is likely to produce a substantially better guideline than one developed in isolation. Rather than relying solely on traditionally reported clinical measures, we can ensure that the outcomes patients care about most are given appropriate weight in the evidence synthesis and in the final recommendations. It is a model that demonstrates how innovation at the level of our national societies, working collaboratively under the EFP umbrella, can elevate the quality and relevance of the guidance we provide to clinicians across Europe and beyond.
"Aesthetics and Patient-Reported Outcomes in Periodontology and Implant Dentistry: ConsensusReport", Journal of Clinical Periodontology, volume 52, issue 9, September 2025, 1222-1244
Biographies

José Nart is professor and chair of the department of periodontology at the International University of Catalonia (UIC) in Barcelona, Spain, where he is also director of the EFP-accredited postgraduate programme in periodontology. He was president of SEPA from 2022 to 2025 and is currently a trustee of the society (2025-2028). Professor Nart is a member of the expert council committee of the Osteology Foundation and is named in Stanford University’s list of the world’s top two per cent of scientists.
Francesco Cairo is professor of periodontology and director of the EFP-accredited postgraduate programme in periodontology and implant dentistry at Florence University, Florence, Italy. He is also director of the postgraduate residency programme in oral surgery and head of the research unit in periodontology and periodontal medicine at the same university. He is the author of the textbook PerioAesthetics as well as more than 120 original articles in international peer-reviewed journals.
David Herrera is dean of the faculty of odontology and professor and chair of periodontology at the Complutense University of Madrid (UCM), Madrid, Spain, where he is also co-director of the EFP-accredited postgraduate programme in periodontology and co-director of the ETEP (Etiology and Therapy of Periodontal and Peri-implant Diseases) research group (UCM). He is chair of the EFP’s workshop committee (2020-2026) and a former president of SEPA (2013-2016).
Moritz Kebschull, who was president of the EFP in 2024-25, holds the chair of restorative dentistry at the University of Birmingham in the UK and an adjunct professorship at Columbia University in New York, USA. He co-chairs the annual EFP workshops and drives the development of high-quality clinical practice guidelines in periodontology and other dental disciplines.




