
Issue No. 147
Summarized from Journal of Clinical Periodontology, Volume 53, Issue 3, March 2026, 394-406
Editor: James Deschner, chair, EFP scientific affairs committee
Peri-implant phenotype influences outcomes of tissue-level implants at five years
Authors: Hamoun Sabri, Parham Hazrati, Lorenzo Tavelli, Carlos Garaicoa-Pazmino, Javier Calatrava, Hom-Lay Wang, Shayan Barootchi
Background
Dental implants are widely regarded as a predictable solution for oral rehabilitation. However, long-term biological stability remains influenced by peri-implant tissue characteristics.
Increasing attention has been directed toward the peri-implant phenotype, which includes mucosal thickness, supracrestal tissue height, keratinised mucosa width, and peri-implant bone thickness. These features may affect marginal bone stability, soft-tissue health and the risk of peri-implant diseases.
Previous evidence suggests that inadequate soft-tissue dimensions—particularly thin mucosa or insufficient keratinised tissue—can predispose implants to mucosal recession and inflammation.
Tissue-level implants have been proposed to enhance peri-implant stability through transgingival healing and reduced micro-gap complications, but longitudinal data relating phenotype to outcomes remain limited.
Aims
To evaluate the association between peri-implant phenotype characteristics and the five-year clinical, radiographic, ultrasonographic, and patient-reported outcomes of soft- tissue-level implants, and to identify potential tissue thresholds linked to peri-implant health.
Materials and methods
- Secondary five-year longitudinal cohort analysis derived from a previous prospective controlled clinical trial.
- In the original study, patients were grouped according to baseline vertical soft-tissue thickness as thin (≤2mm) or thick (>2mm). For the five-year analysis, all available patients were pooled into a single cohort. Twenty-five patients with 25 implants completed the final follow-up.
- At the five-year visit, a blinded examiner recorded probing pocket depth, mucosal recession, keratinised mucosa width, modified plaque index, bleeding on probing, and suppuration. Baseline buccal and vertical soft-tissue thickness measurements from the original trial were also included.
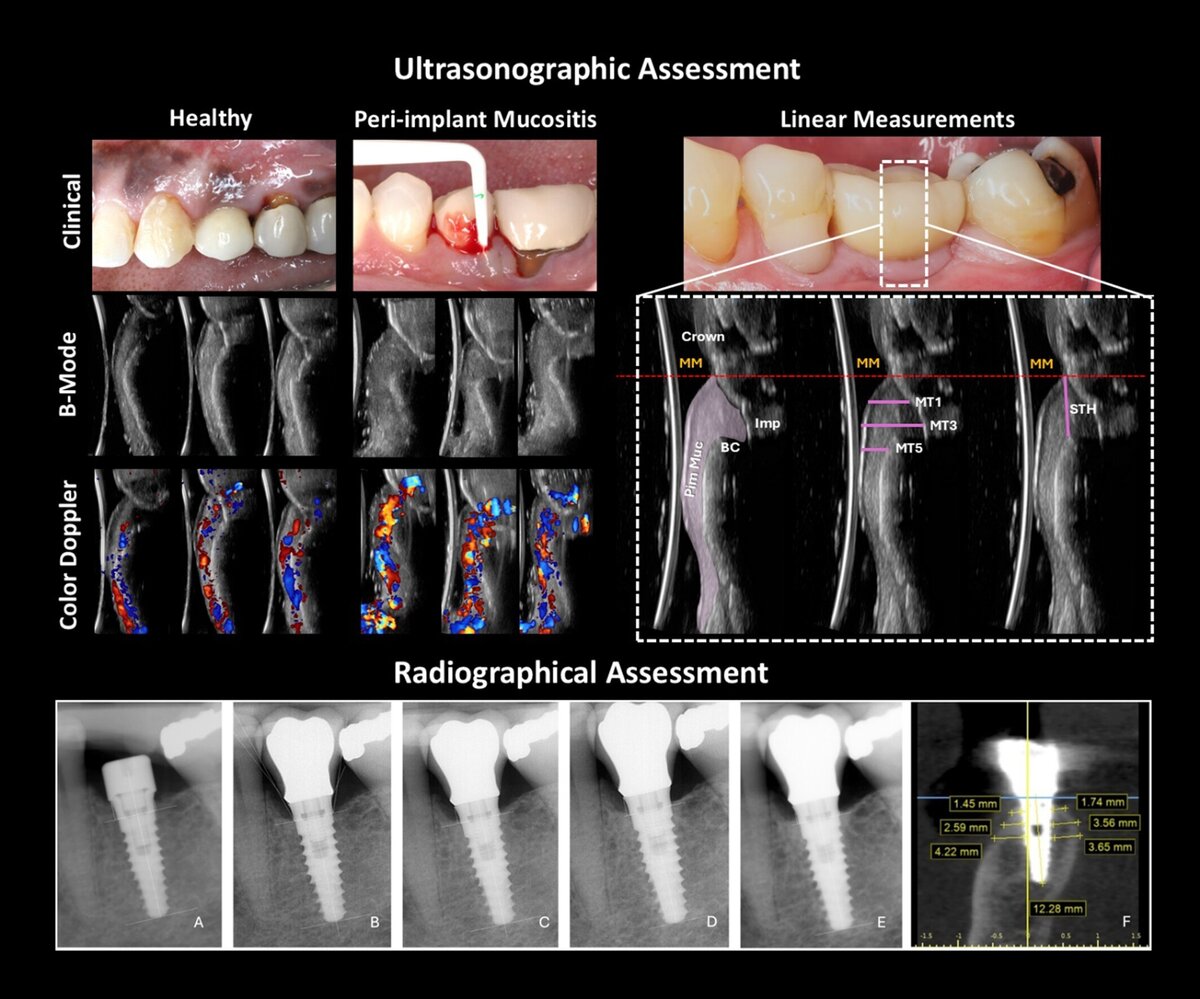
- Radiographic evaluation with standardized periapical radiographs and cone-beam computed tomography (CBCT) for bone thickness and emergence angle.
- Ultrasonography was performed by a blinded, calibrated examiner to measure mucosal thickness, supracrestal tissue height, and tissue perfusion.
- Patient-reported outcomes were assessed using visual analogue scale (VAS) satisfaction, aesthetics, function, and Oral Health Impact Profile-14 (OHIP-14).
- Primary outcomes were peri-implant disease status and implant survival. Secondary outcomes were marginal bone-level changes, peri-implant mucosal recession, patient-related outcomes, and ultrasonographic tissue perfusion.
- Associations were analysed using logistic and linear-regression models.
Results
- Implant survival at five years was 100%, with 64% of implants classified as healthy and 36% presenting peri-implant mucositis, while no peri-implantitis cases were detected.
- Mean marginal bone loss from year one to year five was minimal (0.29 ± 0.29mm), while the total change from crown delivery to five years was 0.56 ± 0.39mm, indicating limited bone changes over time.
- Baseline buccal soft-tissue thickness below 1.5mm and higher plaque scores were significantly associated with mucositis, whereas greater buccal bone thickness, mucosal thickness, and supracrestal tissue height showed protective effects.
- Mucosal recession was significantly linked to baseline buccal soft-tissue thickness below 1.5mm and keratinised-mucosa width below 2mm.
- Ultrasonography demonstrated markedly higher blood flow in diseased implants, strongly correlating with disease status.
- Patient satisfaction was high. Mean overall satisfaction was 88.2% and 90% of patients reported satisfaction scores in the 75% to 100% range. OHIP-14 scores were generally low, suggesting minimal daily-life impact.
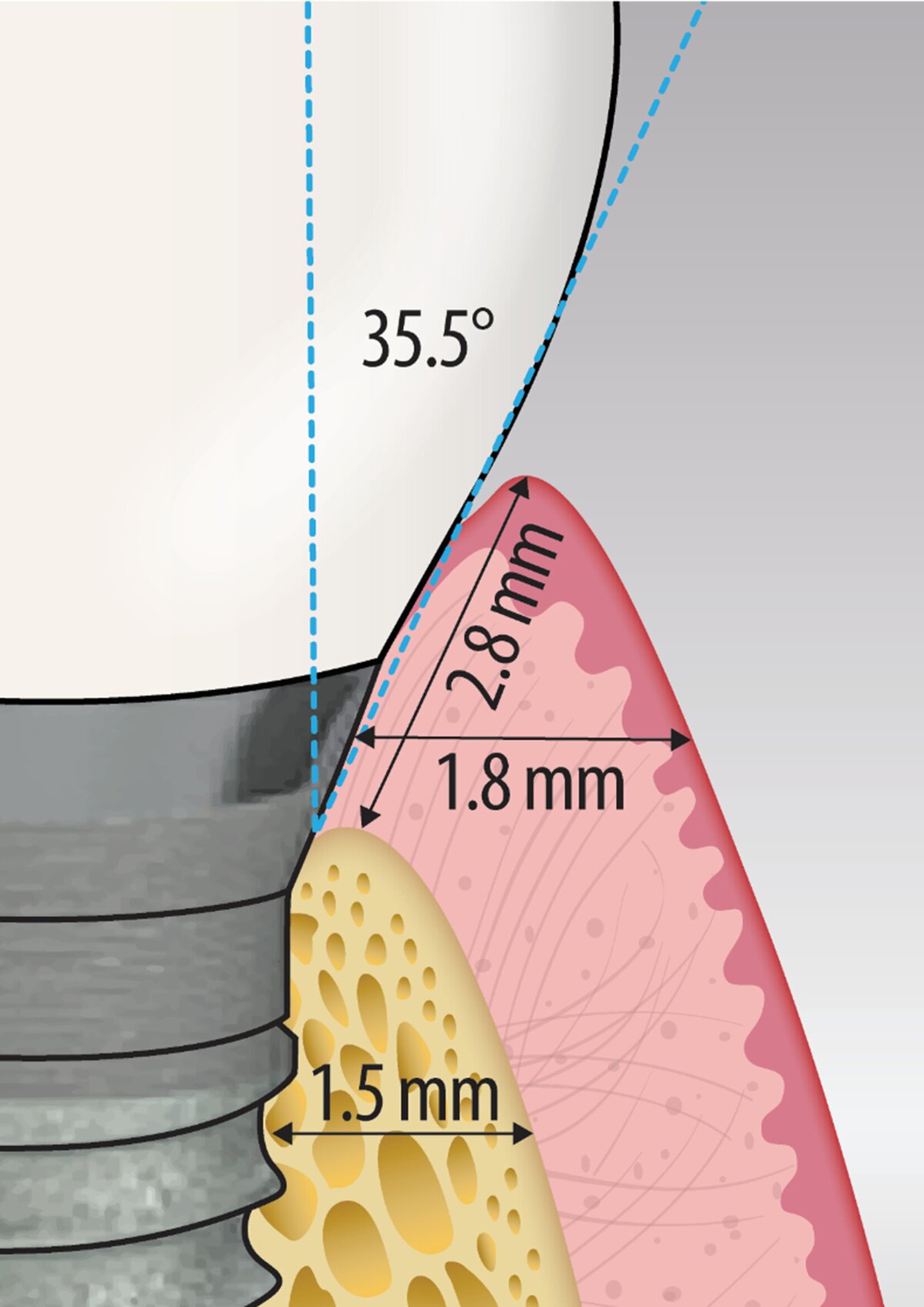
- Receiver operating-characteristic analysis suggested exploratory thresholds associated with long-term health: emergence angle ≤35.5°, buccal bone thickness ≥1.5mm, baseline buccal soft-tissue thickness ≥1mm, mucosal thickness ≥1.8mm, and supracrestal tissue height ≥2.8mm.
Limitations
- Small sample size limits generalizability.
- Single implant system restricts external validity.
- Emergence angle showed potential relevance, but it was excluded from the adjusted multivariable model because of collinearity, and it should therefore be interpreted cautiously.
- The emergence profile was assessed in two dimensions, which may not fully capture clinically relevant three-dimensional contour variation.
- All patients received at least some supportive care, which may have contributed to favourable outcomes and may limit applicability to poorly compliant populations.
Conclusions and impact
- Tissue-level implants demonstrated excellent five-year survival with limited marginal bone changes and high patient satisfaction.
- Peri-implant phenotype parameters were significantly associated with peri-implant health.
- Thin baseline buccal soft tissue and increased plaque were linked to peri-implant mucositis, whereas greater buccal bone thickness, greater mucosal thickness, and greater supracrestal tissue height were linked to healthier peri-implant conditions.
- Greater mucosal thickness, supracrestal tissue height, and buccal-bone thickness were protective.
- The threshold values proposed in this study should be regarded as exploratory and hypothesis-generating, but they may help guide future clinical monitoring and research.
This study suggests that peri-implant tissue dimensions should be considered carefully when planning and monitoring tissue-level implant therapy. Adequate mucosal thickness, keratinised mucosa, supracrestal tissue height, and buccal bone support may help reduce mucositis, recession and bone changes, improving medium- to long-term implant stability.
Rapporteurs: Manal Sarsri Reffassi, Youssra Abarchan, Fares Al Hajeb, Maria Ioanna Alegra, Nicolás Padrós Creus, and Alexa Varela Sarfati, supervised by Prof. José Nart, Prof. Cristina Vallès, Gonzalo Blasi, and Neus Carrió.
Affiliation: Postgraduate programme in periodontology, UIC (International University of Catalonia), Barcelona, Spain
With kind permission from Wiley Online Library. Copyright © 1999-2026 John Wiley & Sons, Inc. All rights reserved




