Clinical & Translational Research, Article
Rethinking bone substitutes in GBR: Can synthetic materials match the standard of care?
20 April 2026
Kiri N. Lang, winner of the first prize in the latest edition of the EFP’s annual Postgraduate Research Prize for preclinical/basic research, describes her research group’s randomized controlled study of bone substitutes in guided bone research and its implications.
Reconstructing lateral bone defects remains one of the key challenges in implant dentistry. While guided bone regeneration (GBR) has become a well-established approach, the choice of grafting material is still evolving. For decades, deproteinized bovine bone mineral (DBBM) has been considered the standard of care. But its limitations—particularly its slow resorption and its animal origin—have driven the search for effective synthetic alternatives.
Against this background, this study aimed to evaluate whether a fully synthetic bone substitute could achieve outcomes comparable to the current clinical standard in GBR. We therefore investigated a novel bilayered biphasic calcium phosphate (BBCP) material designed to mimic natural bone. It consists of an α-tricalcium phosphate (TCP) core with a nanocrystalline hydroxyapatite (HA) coating (approximately 90% α-TCP and 10% HA), which aims to balance stability and resorption.
To evaluate this, we used a standardized preclinical model of lateral bone defects in six beagle dogs, with four defects created in the maxilla of each animal. These defects were intentionally designed as critical-size defects with limited self-healing capacity, allowing us to assess the true regenerative potential of the materials. A critical-size defect model was chosen because such defects do not heal spontaneously and therefore provide a standardized setting to assess the effectiveness of regenerative interventions; in this study, defects of approximately 10 × 8 × 6mm were created.
Four treatment modalities were compared:
- BBCP alone (T)
- DBBM as a positive control (PC)
- A 1:1 combination of both materials (M)
- An untreated negative control (NC)
All defects were treated according to the principles of GBR using a resorbable membrane. After a healing period of 11 weeks, the animals were sacrificed and the samples were analysed using micro-computed tomography (micro-CT) and histological methods (Figure 1).
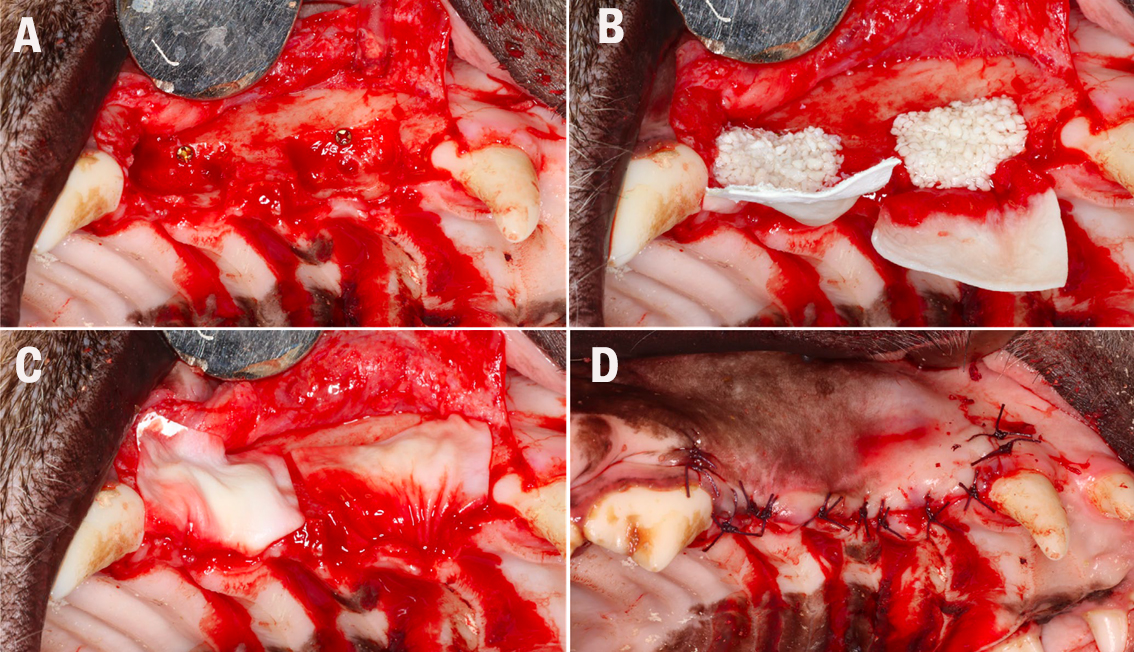
(B) Defect filling according to the treatment modalities. (C) Coverage of the
augmentation area with resorbable barrier membranes. (D) Primary wound closure and
suturing.
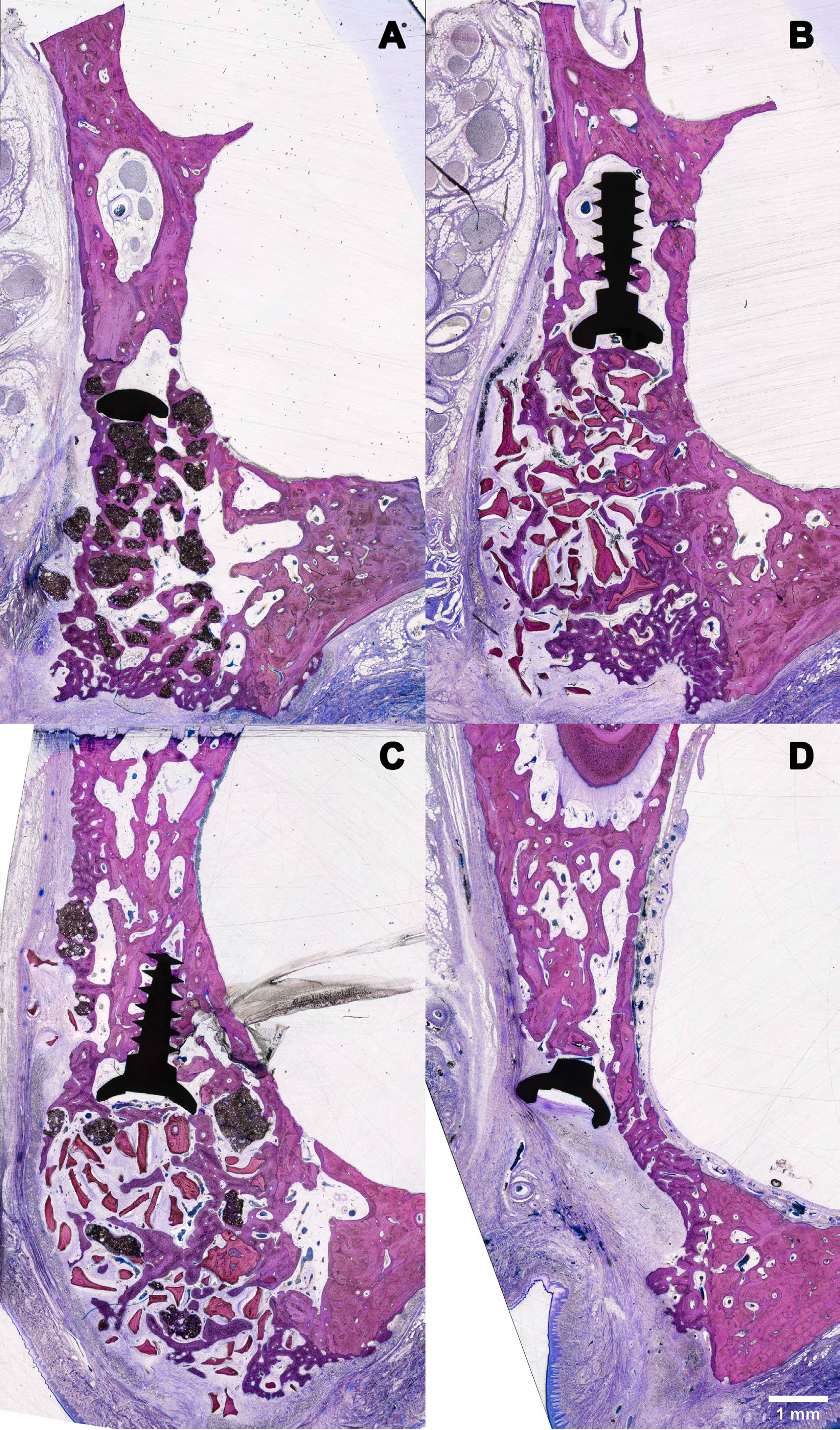
Magnification 4×. OB: old bone; NB: new bone; *: BBCP; #: DBBM; arrowhead:
collagen membrane; S: screw; MS: maxillary sinus.
Overall, the results were highly encouraging. Micro-CT analyses showed that grafted defects exhibited a greater regenerated volume compared to untreated sites, largely independently of the specific biomaterial used. In addition, grafted areas consistently demonstrated a significantly higher proportion of mineralized tissue than non-grafted defects. Histological analysis supported these findings, showing extensive new bone formation in contact with the biomaterials, with a higher bone-to-biomaterial contact for BBCP compared to DBBM, while some DBBM particles were partially surrounded by connective tissue (Figures 2-4).
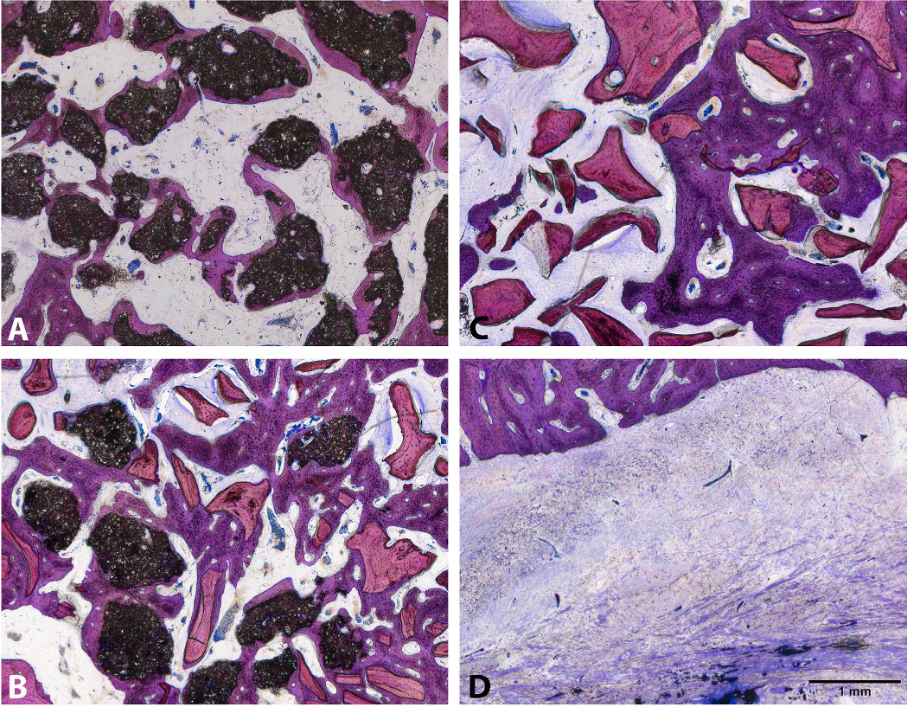
control sites. A: T, B: M, C: PC, D: NC; NB: new bone; *: BBCP; #: DBBM.
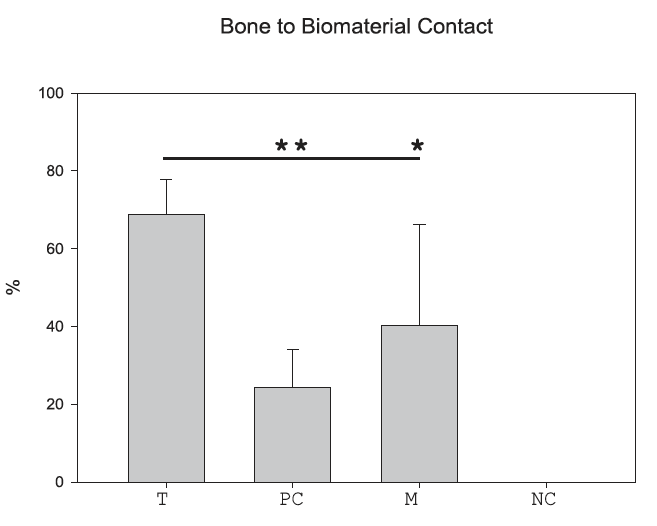
values (%) of bone to mionaterial contact (*< 0.05, **< 0.01, #< 0.001).
From a clinical perspective, these findings suggest that synthetic bone substitutes such as BBCP may represent a viable alternative to xenogeneic materials in guided bone regeneration. They avoid animal-derived components and may offer advantages in availability and cost.
However, caution is warranted. The present study reflects a single healing time point in a preclinical model. Long-term outcomes, as well as performance in chronic defects and clinical settings, remain to be investigated. Future studies should therefore focus on different healing intervals, larger sample sizes, and ultimately clinical trials to confirm these promising results.
Biography

Kiri N. Lang graduated with honours in dentistry from the University of Bern, Switzerland, where she also obtained her Dr. med. dent. degree. She holds a master’s degree in periodontology and implant dentistry and completed the EFP-accredited postgraduate programme at the same institution, becoming a certified specialist in periodontology. Following her training, she spent one year as a research scholar in oral microbiology at the University of Michigan School of Dentistry in Ann Arbor, USA.




