Therapy, Treatment, Article
How the perio-ortho synergy can improve smile aesthetics
14 March 2023
The EFP Perio Master Clinic 2023 took place in Antwerp, Belgium, on 3-4 March focusing on “the Perio-Ortho Synergy”. One of the sessions focused on how collaboration between periodontists and orthodontists can enhance smile aesthetics. Session moderator Bruno de Carvalho, and speakers Belén Solano-Hernández, Óscar González-Martín, and Antonio Liñares offer their perspectives.
The synergy between perio and ortho is without doubt an excellent example of the success of multidisciplinary approaches in dentistry, writes Bruno de Carvalho. In aesthetic dental treatments, a correct orthodontic and periodontal diagnosis and a thorough analysis of the hard and soft tissues are of crucial importance to obtain long-term results in such a demanding sector.
This multidisciplinary approach is often demanded because aesthetic sequalae are one of the common consequences of periodontal disease. For this reason, understanding both the biological basis of periodontal surgical procedures and the basis of orthodontic movements can provide clinical results of excellence in the aesthetic area.
This session at Perio Master Clinic 2023 allowed participants to see how, in practice, this perio-ortho synergy can bring more harmonious aesthetic results and long-term stability at both hard and soft tissues. Experienced periodontists and orthodontists took us on a journey through complex aesthetic clinical cases with all the steps and clinical decisions that were involved in their execution.
Leveraging orthodontic extrusion in clinical practice
By Belén Solano-Hernández and Óscar González-Martín
Orthodontic forced extrusion (OFE) is an orthodontic tooth movement in a coronal direction to modify the tooth position and/or induce changes on the surrounding bone and soft tissue with a therapeutic objective. The evidence emanating from clinical reports and case-series studies indicates that OFE is a predictable treatment option that can be used to manage a variety of clinical situations.
Common indications include:
- Traction of impacted teeth.
- Exposure of teeth presenting structural damage, to facilitate restorative therapy.
- Treatment of periodontal bony and papillary defects.
- Development of the implant site.
Modern applications of OFE include the modification of the soft-tissue envelope to correct an inadequate gingival zenith position and papillary deficiencies between two teeth or between a tooth and an existing implant. Unfortunately, there is a lack of established protocols and guidelines for the application of this technique in clinical practice.
Historically, two protocols have been proposed to apply to OFE: so-called “rapid” and “slow” eruption. However, there are no universal parameters that define the two procedures, as there are multiple variables that may play a role in the selection of a specific protocol for tooth movement. The total time of active orthodontic extrusion is primarily influenced by the clinical protocol applied – the magnitude of the orthodontic force applied and whether circumferential supracrestal fiberotomy (CSF) or intermediate tooth stabilization (ITS) are performed – the amount of tooth extrusion desired, and root morphology.
There is also controversy regarding the use of tooth-stabilisation protocols during and upon completion of orthodontic movement. It thus seems that “rapid” and “slow” are largely unsubstantiated descriptors that have been used indiscriminately to characterise a variety of extrusive movements, regardless of whether or not CSF and ITS are involved.
In our presentation at Perio Master Clinic 2023, we provided a concise perspective on orthodontic extrusion by discussing key biological principles and technical aspects, which we have translated into guidelines for the management of different clinical scenarios that define three different clinical protocols:
- OFE with CSF and without ITS.
- OFE without either CSF or ITS.
- OFE without CSF and with ITS
Table: Three clinical protocols for orthodontic forced exclusion
Protocol | Aim | Biological rationale | Clinical protocol | Indication(s) |
OFE with CSF and without ITS | Tooth extrusion, with no modification of periodontal tissues | Uninterrupted tooth extrusion avoiding elongation of periodontal fibres to prevent tension on the gingiva and crestal bone | Forced extrusion applying heavy forces with periodic severance of supracrestal periodontal fibres and root planing, and without intermediate tooth stabilisation | Expose subgingival / subcrestal tooth structure to facilitate restorative therapy |
OFE without CSF or ITS | Tooth extrusion, with traction of gingival tissues and minimal or no alveolar bone changes | Uninterrupted rapid tooth extrusion with intentional elongation of periodontal fibres Note: This approach may cause sulcular epithelium eversion and a subsequent recession defect | Forced extrusion applying heavy forces with no fiberotomy and without intermediate tooth stabilization Note: A longer stabilisation period after completion of tooth movement is usually required with this approach | (1) Modification of the soft-tissue envelope (2) Implant-site development |
OFE without CSF but with ITS | Tooth extrusion, with traction of both gingival tissues and alveolar bone | Elongation of periodontal fibres with interrupted tooth extrusion to allow reorganization of the supracrestal gingival fibres and bone apposition Note: This approach rarely causes sulcular epithelium eversion and a subsequent recession defect | Forced extrusion applying light forces with no fiberotomy and with periods of intermediate tooth stabilisation | (1) Management of impacted teeth (2) Treatment of periodontal infrabony defects (3) Modification of the soft-tissue envelope (4) Implant-site development (5) Tooth extraction when a surgical protocol is contraindicated |
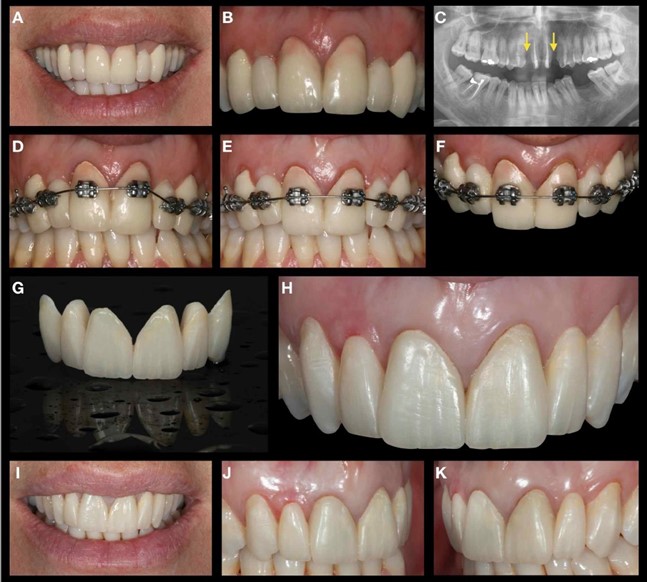
Note: A & B: Initial clinical presentation. Note the agenesia of both lateral incisors, the mid-buccal recession on both central incisors, and the poor aesthetics of the existing restoration. C: Orthopantomography. Note the root-canal treatment of the central incisors and loss of interproximal bone on the distal aspect of both teeth. D & E: OFE was done for two months. F: Initiation of the stabilisation process, which lasted three months. Note the marginal "red patch”, which is indicative of eversion of the sulcus. G: Provisional restoration. H, I, J & K: Final insertion of the provisional restoration.
Article adapted from: Oscar González-Martín, Belen Solano-Hernandez, Ana González-Martín, Gustavo Avila-Ortiz ‘Orthodontic Extrusion: Guidelines for Contemporary Clinical Practice’. Int J Periodontics Restorative Dent. 2020 Sep/Oct;40(5):667-676. doi: 10.11607/prd.4789.
‘The patient wants to smile’
By Antonio Liñares
Mucogingival surgery helps us both to restore the aesthetics of the smile and improve the support of the teeth and thus their long-term maintenance. Classic and new techniques can be used with slight modifications in situations of advanced recession. In addition, interdisciplinary treatments can help us to treat these complex recessions to achieve success in treatment.
My presentation at Perio Master Clinic 2023 showed a new interdisciplinary protocol for the treatment of Class 3/RT2 recessions in the anterior teeth of periodontal patients.
When we treat periodontal patients, we are dealing with patients with aesthetic sequelae resulting from black triangles. Moreover, after the disinfection phase, soft-tissue shrinkage is expected, which impairs patients’ aesthetics. We may be successful in treating the periodontal disease, but the patient may be unhappy because of the aesthetic sequelae. Professor Raúl Caffesse always used to say, “the tooth wants to live”, to which I would add, “the patient wants to smile.”
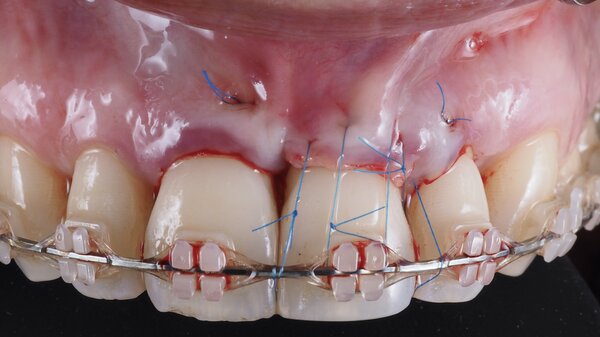
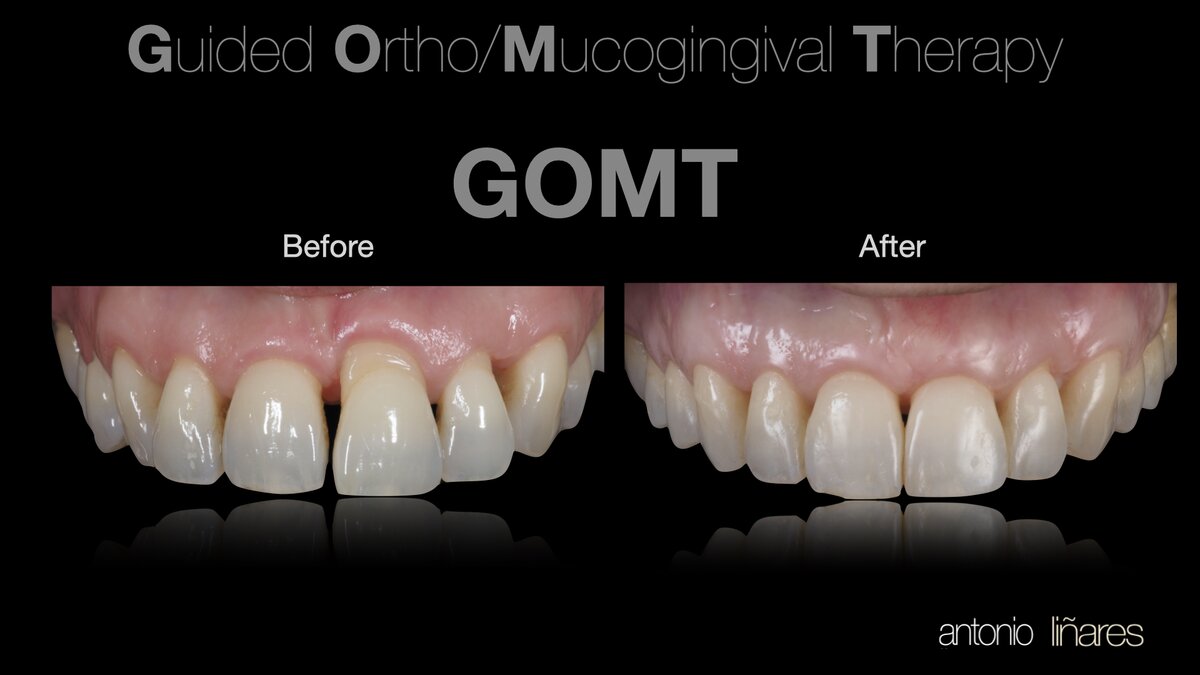
This innovative protocol consists in performing mucogingival surgery with a tunnel connective-tissue graft during orthodontic tooth movement – not before or after, but during. I have named this approach the Guided Ortho Mucogingival Therapy (GOMT) protocol, because we are moving the tooth with a connective-tissue graft aiming at root coverage, not only buccal but also mesial and distal where the black triangles are present.
This orthodontic tooth movement is intrusion and palatal torque of the root, similar to what occurs with the biologically oriented preparation technique (BOPT) concept. The idea is to leave space for the soft tissues to advance coronally, but first thickening them.
The session on “The ortho-perio synergy to enhance smile aesthetics” at Perio Master Clinic 2023, took place on Friday 3 March. In addition to the topics addressed above, the session also included a lecture by orthodontist Nuno Sousa Dias on “Orthodontics for smile aesthetic space management”.

Biographies
Bruno de Carvalho is a periodontist, PhD fellow, and head of clinic at the EFP-accredited postgraduate programme in periodontology at the University of Liège in Belgium. He is is the regular chair of the EFP Perio Talks podcasts and a member of the federation's communications committee.

Belén Solano-Hernández works in a private practice exclusively in orthodontics. She received her master’s degree in orthodontic and dentofacial orthopaedics from the University of Seville, Spain, in 2009 and subsequently trained in the orthodontic department of the University of Geneva in Switzerland.

Óscar González-Martín teaches at the EFP-accredited postgraduate programme in periodontology at the Complutense University of Madrid in Spain and has a private practice exclusively dedicated to periodontology, prothesis, and implants. He obtained his international PhD from the University of Seville in 2015.

Antonio Liñares is associate professor of periodontology at the University of Santiago de Compostela in Spain and has a private practice in A Coruña limited to periodontology and implant dentistry. He has a European PhD with honours from the University of Santiago de Compostela and received his master’s degree in periodontology from the EFP-accredited programme at UCL Eastman Dental Institute in London, UK.




